Polycystic Ovarian Syndrome
Polycystic ovary syndrome, known as “PCOS” for short, is a condition where the ovaries produce abnormal amounts of androgens. These male sex hormones are usually only present in small amounts in women. Polycystic ovary syndrome was named to illustrate the small cysts that form in the ovaries. Some women with PCOS are on a case-by-case basis, and some women will form cysts while others will not. Women with polycystic ovary syndrome often will not ovulate as they do not make enough of the needed hormones. When ovulation does not occur, many women will then develop small cysts. Since women with PCOS have high levels of androgens, it interferes with the women’s natural menstrual cycle and can cause many other symptoms of PCOS.
Polycystic ovary syndrome’s exact cause is unknown but can be linked to several other conditions. Insulin resistance is often linked to PCOS because when the insulin levels build up, it causes cause a higher androgen level. Obesity can also contribute to increasing insulin levels, which could worsen someone’s PCOS symptoms. Other causes and risks could be having a family history of PCOS. It’s common for sisters or mother and daughter to present with PCOS, especially if they have insulin resistance or are obese.
There is a wide range of symptoms associated with polycystic ovarian syndrome. That being having irregular or light menstrual cycles or even missing them altogether. Excess body hair, including chest, stomach, and back hair, is more common in men than women naturally—weight gain, primarily in the abdomen and skin tags around the neck and armpits. Often the back of the neck, the armpits, and underneath the breast will be patches of much darker and thicker skin. Women will also present with acne, excessive oily skin, thinning hair, or male-patterned baldness. Along with what was discussed early are ovaries with many cysts or larger ones. Lastly, many women dealing with polycystic ovarian syndrome also struggle with infertility.
Polycystic ovarian syndrome is diagnosed through a series of exams. They typically start with a medical history and symptoms present, to a physical exam which likely includes a pelvic exam. These exams aim to check the health of the women’s reproductive organs, both internally and externally. Typically ultrasounds will be taken to check out the ovaries and identify if there are any cysts present. Additionally, they may check the thickness of the endometrium. Along with this, a blood test will be run to look for high levels of androgens and other hormones.
Treatment options are available, but this disorder is not curable. Treatments can range depending on the women’s age, the severity of symptoms, overall health, and the possibility of wanting children in the future. In the cases a woman plans to become pregnant, treatments will consist of implementing a healthy diet and physical activity to lose weight to help alleviate some symptoms; this is an overall good option either way. Both help the efficiency of insulin and blood glucose levels and ovulation. Another option is medication, which may help with ovulation. If a woman is not planning to become pregnant, the options include birth control pills which will help control the menstrual cycles, lower androgen levels, and reduce acne. As well as diabetes medical to help lower insulin resistance and androgen levels. As well as, if a woman is
Complications can arise with polycystic ovarian syndrome as it can cause other health issues for a woman. This could be type 2 diabetes, high blood pressure, corbels associated with the heart and blood vessels, and the development of uterine cancer. Often, a woman’s biggest struggle with PCOS is infertility.
References
John Hopkins Medicine. (2023). Polycystic Ovary Syndrome (PCOS). Johns Hopkins Medicine. Retrieved August 1, 2023, from https://www.hopkinsmedicine.org/health/conditions-and-diseases/polycystic-ovary-syndrome-pcos
Mayo Clinic. (2022, September 8). Polycystic ovary syndrome (PCOS) – Symptoms and causes. Mayo Clinic. Retrieved August 1, 2023, from https://www.mayoclinic.org/diseases-conditions/pcos/symptoms-causes/syc-20353439
National Library of Medicine. (2022, January 17). Polycystic Ovarian Disease. NCBI. Retrieved August 1, 2023, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8775814/thoroughly,%20reviewing%20the%20related%20clinical%20trials%20over%20the%20past%20five%20years.

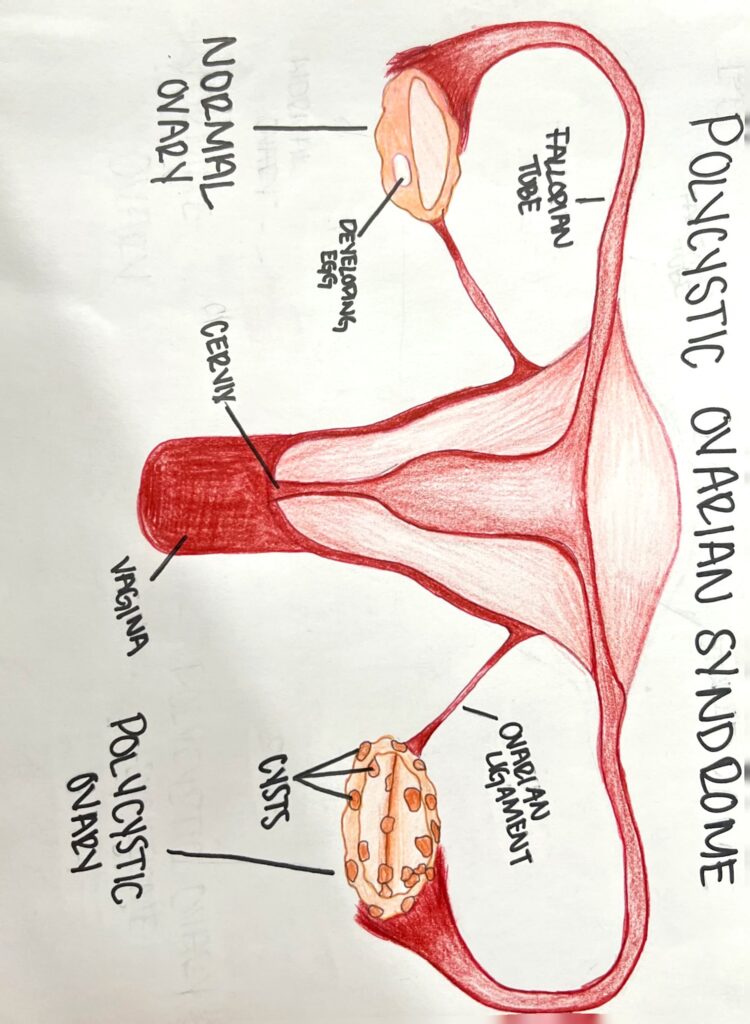
For Kenna Marchesseault’s STEAM project, she discusses polycystic ovarian syndrome (PCOS). The condition involves an overproduction of male sex androgens and only affects a minute amount of women. PCOS involves the growth of small cysts on the ovaries and causes most women with the condition to not ovulate. The lack of ovulation is what causes these cysts. The high levels of androgens also cause interference with menstruation as well as abnormal hair growth. Some women’s menstrual cycles will be irregular, light, or missed on a month-to-month basis. Infertility, acne, thinning of hair, skin tags, and dark skin patches are other symptoms seen with PCOS. Obesity can also contribute to worsening symptoms due to high insulin levels. The condition can be hereditary and is common for sisters, mothers, and daughters to have PCOS if there is a history. It is diagnosed through pelvic exams where reproductive organs of the internals and externals are checked including the endometrium for thickness. Ultrasound can help to identify any cyst development and see ovary health. Blood tests can assist in identifying androgen levels. Unfortunately, there is no cure for this condition but there are treatment options. These treatment options include dietary changes and physical activity to lose weight and help correct insulin and blood glucose levels. This is a good option for women aiming for pregnancy. Other treatment options are medications such as birth control to help with the menstrual cycle, acne, and lower androgen levels. Kenna’s media is a drawn photo showing parts of the female reproductive system and where cysts will be found on the ovaries.