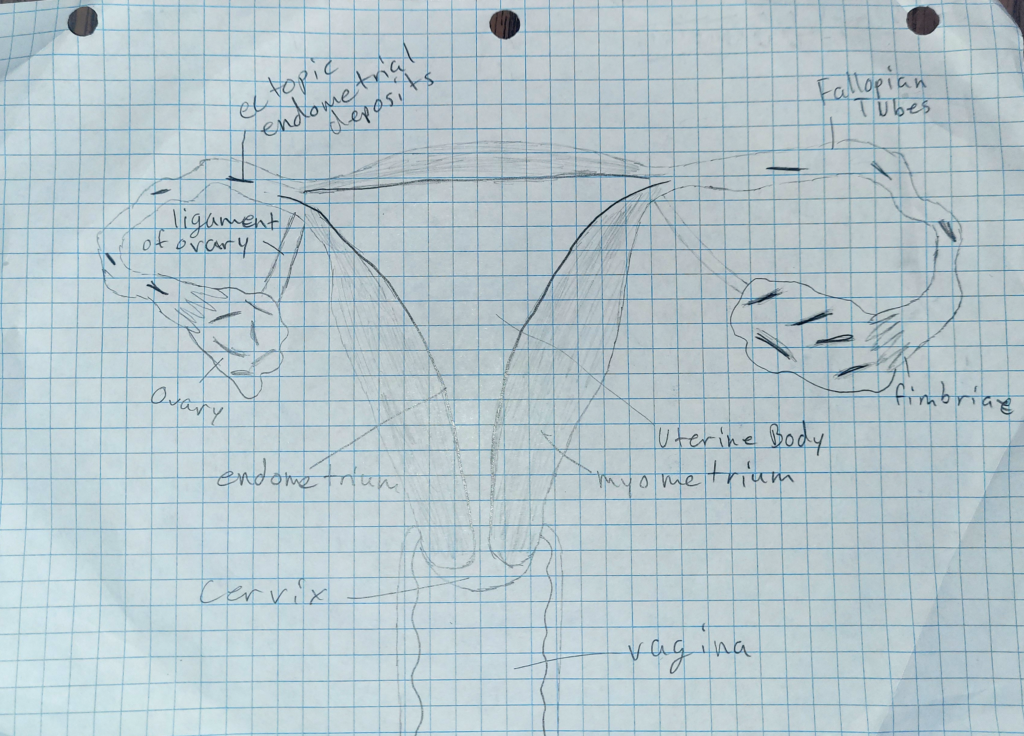
The female reproductive system is made up of many parts, the most commonly known uterus, fallopian tubes, and ovaries. The breasts are also a part of the system, and play an important role post childbirth, with providing colostrum and then milk to the infant. When the ovaries release an egg, it travels through the fallopian tubes, where it can be fertilized, and then into the uterus, where it will implant if fertilized into the uterine lining, or endometrium. A disease that is not very common, and even less talked about is endometriosis. Endometriosis is where cells such as those in the endometrium grow outside of the uterus. They can be found on the ovaries, fallopian tubes, the exterior of the uterus, the ligaments around the uterus, the lining of the pelvic cavity, and in the space between the uterus and rectum or bladder. Less commonly, it can also be found on the bladder, the cervix, intestines, and the vagina or vulva. This external endometrial tissue does not shed during the menstrual cycle, and can lead to inflammation, and even cysts and scarring. It can also cause adhesions, which is when fibrous tissue build up between organs, causing them to stick together.
Doctors don’t know what causes endometriosis, but there are many theories, including endometrial cells being transported through the lymph or blood systems, genetics, transplantation after surgeries such as c-sections or hysterectomies, and reverse menstruation, where the endometrial tissues enter the fallopian tubes and abdomen instead of exiting the body during the period. Some common symptoms in people with endometriosis are painful menstrual cramps that may got into the stomach area and back, pain during or after sex, diarrhea or constipation during menstruation, fatigue, irregular or heavy periods, painful urination or bowel movements during menstruation, and spotting or bleeding between menstrual periods.
Endometriosis is also theorized to cause infertility, though a clear cause-effect connection is still debated heavily. In healthy patients, the menstrual debris is destroyed by macrophages specifically targeting inflammation. However, in endometriosis patients, these macrophages are overabundant, which is allowed by several defective cells types, such as the T helper, natural killer, and cytotoxic T cells. Lending to the theory that endometriosis can cause infertility, the imbalance in peritoneal fluid and sever inflammation can decrease endometrial receptiveness to embryo implantation. Other endocrine and ovulatory abnormalities have been seen, such as Luteinized Unruptured Follicle syndrome, irregular follicle growth, and premature luteinizing hormone peaks. Many studies suggest that changed implantation methods may be the basis of infertility that is associated with peritoneal endometriosis.
Endometriosis is uncurable and is most commonly treated by reducing the estrogenic stimuli, which encourage ectopic endometrial growth, along with surgery to remove the lesions, or a complete hysterectomy. Endometriosis risk is significantly higher if the mother has polycystic ovary syndrome, as it is mediated through testosterone use, and prenatal exposure to diethylstilbestrol, bisphenol, or exposure to relatively high levels of phthalates. There is a theory that endometriosis is a direct opposite disease to PCOS, which heavily influences the diagnosis, treatment, prevention and further research.
Endometriosis affects so many people, men and women, that it should be a more pursued topic, especially in the treatment department. So while endometriosis is not typically a fatal disease, it is very uncomfortable, and often painful to live with, and treatments are less than ideal, especially without a cure.
Works Cited
Johns Hopkins Medicine. (2023) Endometriosis https://www.hopkinsmedicine.org/health/conditions-and-diseases/endometriosis. Accessed 26 April 2023.
Coccia, M. E., Nardone, L., & Rizzello, F. (2022). Endometriosis and Infertility: A Long-Life Approach to Preserve Reproductive Integrity. International Journal of Environmental Research and Public Health, 19(10), 6162. MDPI AG. Retrieved from http://dx.doi.org/10.3390/ijerph19106162. Accessed 26 April 2023.
Dinsdale, N., Nepomnaschy, P., Crespi, B. (2021). The evolutionary biology of endometriosis, Evolution, Medicine, and Public Health, 9(1), 174-191. https://doi.org/10.1093/emph/eoab008.