Achalasia is a rare disorder that results from progressive destruction of the ganglion cells in the myenteric plexus esophageal wall. The distraction of the cell leads to the inability of the lower esophageal sphincter to relax and leads the loss of peristalsis of the distal esophagus.
As a result there is dilation of the distal esophagus, patients will often present with dysphasia, regurgitation, heart burn reflux and weight loss and can occur to anyone between the ages of 25-60 years of age. There’s a lot of misdiagnosis’s made in patients, and they’re normally diagnosed with gastrointestinal reflux rather than Achalasia. Patients with achalasia often present with dysphasia occurring with both solids and liquids along with non-acidic regurgitation of undigested food, additional symptoms include heartburn weight loss and chest pain unresponsive to acid reducing agents.
Now the esophagus is a muscular tube that transports swallowed solids and liquids from the pharynx to the stomach. The suffix has a similar structure to the rest of the gastrointestinal tract as it consists of outer layer of connective tissue, the adventitia to muscular layers and other longitudinal layer and an inner circular layers, a submucosa, a mucosa consistent of non-keratinized stratified squamous epithelium which is continuous with the columnar epithelium of the stomach.
The gastrointestinal tract Is able to move food along and not backwards through its intrinsic peristaltic movement. The intrinsic peristaltic movements are controlled by the enteric nervous system which is composed of an outer plexus (the myenteric plexus also known as the Auerbach’ plexus), and then there inner submucosal plexus also known as the meissner’s plexus.The myenteric plexus lies between the longitudinal and circular muscle layers of the gut and exerts main control over gastrointestinal movement. The inner mucosa plexus, the meissner’s plexus is the main control of gastrointestinal secretion and local blood flow.
There are two esophageal sphincter, an upper and lower one, the lower esophageal sphincter is a muscle and it’s tone is controlled by the myenteric plexus. The myenteric plexus consists of excitatory nerve cells, which contract the sphincter, preventing reflux of food and acids from the stomach, it also contains inhibitory nerve cells, which relaxes the psych inter when food/ water travels down the esophagus to the stomach. I should also mention, the enteric nervous system is partly controlled by the central nervous system, the vagus nerve from the brainstem innervates the enteric nervous system and so do the sympathetic nerve fibers from the spinal cord.
The pathophysiology of Achalasia is thought to be the result of loss of the inhibitory neurons in the myenteric plexus of the distal esophagus and the lower esophagus sphincter, that leads to unmatched excitation. The excitatory cells in the myenteric plexus release the neurotransmitter acetylcholine which causes smooth muscle contraction of the distal esophagus and the lower esophageal sphincter. Usually the inhibitory cells release vasoactive intestinal peptide (VIP) and nitric oxide, which have the effect of smooth muscle relaxation, however in the absence of vasoactive intestinal peptide and nitro oxide due to inhibitory cell destruction. Acetylcholine from the excitatory neurons is unmatched, and the result of this imbalance is the failure of the lower esophageal spnichter to relax due to uninhibited contraction and loss of distal esophageal peristalsis.
Achalasia is also considered to be an immune disorder, Patients with Achalasia have been shown to have antibodies to myenteric in their circulation. So the exact etiology of Achalasia is unknown, however it is thought that it can be due to idiopathic unknown cause, associated with viral parasitic infections, autoimmune or neurodegenerative disorders.
Approaches to treatment of Achalasia include endoscopy or surgical intervention .
References;
https://www.mayoclinic.org/diseases-conditions/achalasia/symptoms-causes/syc-20352850
https://www.ncbi.nlm.nih.gov/books/NBK519515/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3793135/
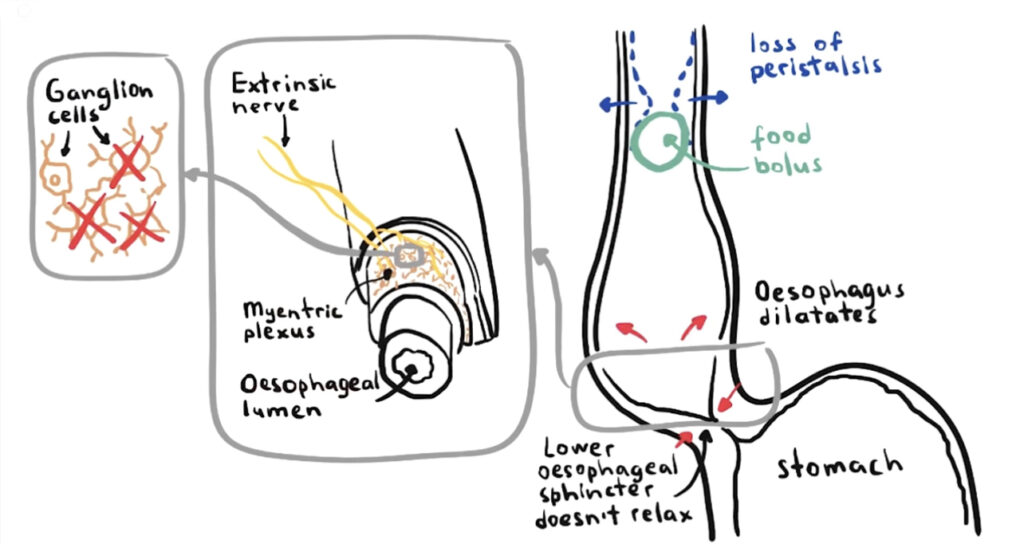

Achalasia is a disorder characterized by regurgitation, heart burn, and unintentional weight loses that is not correlated to gastrointestinal reflux. The project here demonstrates the anatomy of achalasia through depicted destroyed ganglion cells in the myenteric plexus surrounding the esophageal lumen. This contributes to a loss of peristalsis in the upper esophageal sphincter and causes the lower sphincter to not relax. The overall cause of achalasia is not known, but may be attributed to autoimmune issues.