For my STEAM project, I chose to examine the effects of neurophysiology and psychology on signaling between nociceptors and the brain and how that creates pain tolerance. This relates in particular to the objective of “explaining how sensory cells translate stimulus into action potentials”. For my media, I am presenting a comic strip that uses a common neuron as a personified character who explains what an action potential is and how it relates to the brain. It will then introduce the pain matrix which consists of a multitude of partnered systems made up of various receptors such as photoreceptors.
The pain matrix is “not a fixed arrangement of structures but rather a fluid system composed of several interacting networks. It includes several regions of the brain that receive input from the body’s nociceptive systems. It then assesses the physical characteristics of the bodily pain” (Garcia-Larrea and Bastuji). While the sensation of pain is received via the nociceptors, the pain matrix is a system that also verifies whether the origin of the pain is real and whether the brain needs to comprehend the stimulation at the given moment. As this is a mostly cognitive function, it is greatly affected by the two distinct ways that we notice pain: from our cognitive awareness and the salience or importance of the stimulation (Legrain et al). This is the reason why anesthetics work for surgery. While the nociceptors are picking up the stimulation that would normally cause pain, the lack of cognitive activity means that the brain can’t pick out these important sensations of pain that would normally tell us we are being cut open. There is no attention and therefore it becomes impossible for the nociceptors to signal the brain to react to the stimulation it is receiving from these important receptors. This is why other receptors such as photoreceptors play a role in the pain matrix system, the visible sight of an injury by a cognitive brain can tell it that it needs to legitimize the nociceptor stimulation that it has been receiving until now to let you know that you are in danger.
This pain matrix system can be affected by a variety of factors, such as level of consciousness and emotion. Level of consciousness as previously discussed is a common example of stopping the pain matrix from identifying pain, however, emotions play a part in this system as well. The chemical and hormonal interference by emotions, while not as strong as being unconscious, can greatly affect the salience of our pain. For example, if we are scared then the pain could become heightened as our body is attempting to take in all sensory information at the given moment. While intense happiness may cause the opposite, blinding us to the pain as adrenaline and dopamine are pumped into our bodies. While this can be very beneficial, allowing us to act in our lives despite chronic pain, overuse can cause many problems. Studies have shown that overutilization of the pain matrix to limit chronic pain can alter the hormonal balances in the brain. This can cause problems such as depression as well as drug addiction to pain killers such as oxycodone in people with long-term chronic pain (Mitsi and Zachariou).
Sources:
Garcia-Larrea, Luis, and Hélène Bastuji. “Pain and Consciousness.” Progress in Neuro-Psychopharmacology & Biological Psychiatry, U.S. National Library of Medicine, 20 Dec. 2018, https://pubmed.ncbi.nlm.nih.gov/29031510/.
Legrain, V., et al. “Cognitive Aspects of Nociception and Pain. Bridging Neurophysiology with Cognitive Psychology.” Neurophysiologie Clinique/Clinical Neurophysiology, Elsevier Masson, 20 July 2012, https://www.sciencedirect.com/science/article/pii/S0987705312002626.
Mitsi, Vasiliki, and Venetia Zachariou. “Modulation of Pain, Nociception, and Analgesia by the Brain Reward Center.” Neuroscience, U.S. National Library of Medicine, 3 Dec. 2016, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5083150/.
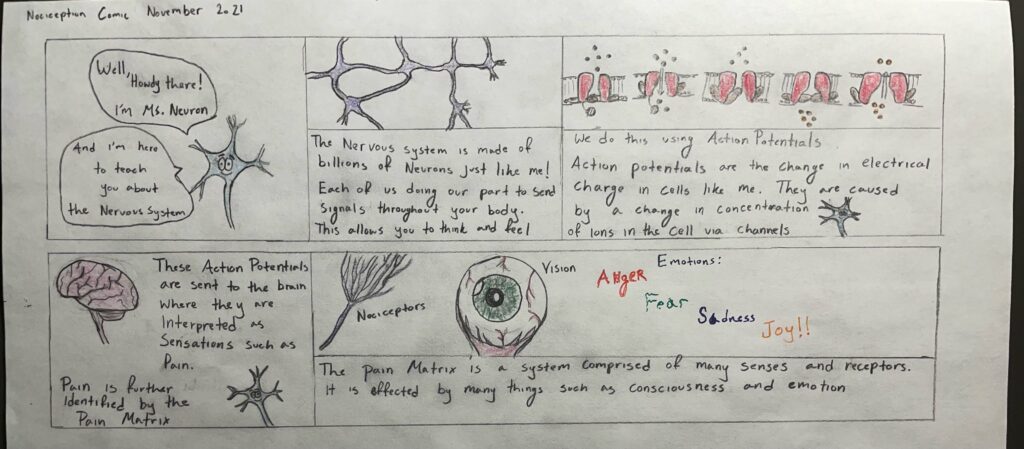

First and foremost, I want to mention that I appreciate you having used a comic strip that you wrote, designed, and drew on as your creative project component for the STEAM project. The reason that I appreciate your use of the comic strip is that comic strips, at least to me, tend to be engaged with a mindset of enjoyment and in a low-stakes environment. These two things help to give the viewer/reader a more accessible approach to the concept that you researched and wrote on in your STEAM project regarding the pain matrix.
The idea of the pain matrix, by the way, is one that was new to me upon first reading and viewing your work. I did not realize that nociceptors are aided by other sensory receptors in the body to communicate signals to the brain to affirm whether or not pain should be perceived. Of course, this makes more sense to me the more I think about it after having the concept introduced as even the idea of watching myself get hurt via a cut or burn sounds more painful than getting cut or burned without looking. Another real world example of this, I think, might be when you go to get a shot from a doctor and how some people look away in order to experience less pain. The example I’ve given might be attributed to the placebo effect, but in the explanation of your work and research you did mention how the psychological and states of consciousness are also incorporated into the pain matrix to work to experience pain in the human body. With that being said, it makes total sense that the placebo effect, in regards to my prior shot example, is definitely a part of the pain matrix too.
Thank you for researching this topic and for sharing what you’ve learned with others. It was a really interesting topic that I was not aware of before interacting with your work and I feel that I grasped the concept well after reading what you had written and seeing what you had made.