
BIPOLAR DISORDER AND THE BRAIN.
There is much we dont understand and still learning about mental health and the effects on the brain, this is especially true for Bipolar disorders. The media’s focus is often negative when it comes to Bipolar disorder. The media often portrays people with this disorder as loose cannons, unpredictable and oftentimes dangerous. The objective of this paper is to showcase the various symptoms present and why they are often confused with other mental health issues as well as the physical changes in the brain when Bipolar Disorder is present.
The truth is, because mental health has been a taboo subject for so long the general public is not informed and has misconceptions as to the onset age of this disorder, relying heavily on the media to base their opinions off of. They are often ignorant of how symptoms may present themselves, how these symptoms affect everyday life. Ignorance is especially true for the understanding of how bipolar disorder affects and changes the brain for those who have been diagnosed.
Understanding mental health has proven tricky. A patient may experience a mild symptom while another experiences that same symptom and on a much larger scale. This is true for most mood disorders. The difference with Bipolar disorder in particular “misdiagnosed with major depressive disorder” and ADD when younger patients start to present symptoms. This in turn leads to misdiagnosis for patients and incorrect treatment. Research has found that Bipolar disorder symptoms may exhibit themselves as early as early to late adolescence. This translates to roughly “28% in adolescence, and 53% at peak ages 15-25.” Because “Manic- depressive illnesses magnifies common human experiences to larger than life proportions. [….] exaggerations of normal sadness and joy.” It is not unreasonable to speculate and categorize these symptoms as normal outbursts of an adolescent going through puberty.
Bipolar symptoms can be but are not limited to; “A dysregulation of mood and associated impulsivity […] and risky behavior.” This behavior can be lack of financial irresponsibility, hypersexuality, risky sexual behavior. As mentioned previously, symptoms exhibited in Bipolar disorder do not have to be volatile in order for a person to have this mood disorder and be accurately diagnosed. Decreased need for sleep and increase in productivity during manic episodes can translate to becoming successful at work and/or school. These two symptoms in particular go unnoticed by both healthcare professionals and the patient themselves. When experiencing a manic or hypomanic (manic episode not as severe) patients do not see the need to seek help or if they have done so due to presenting themselves as happy, productive and motivated individuals, healthcare professionals often dismiss the depressive episodes experienced before as situational.
We now have a basic understanding of what Bipolar Disorder looks like, the symptoms and how those symptoms translate to everyday life. The question now begs, what is happening in the brain of those who are diagnosed with Bipolar Disorder that differs from those who do not suffer from mood disorders?
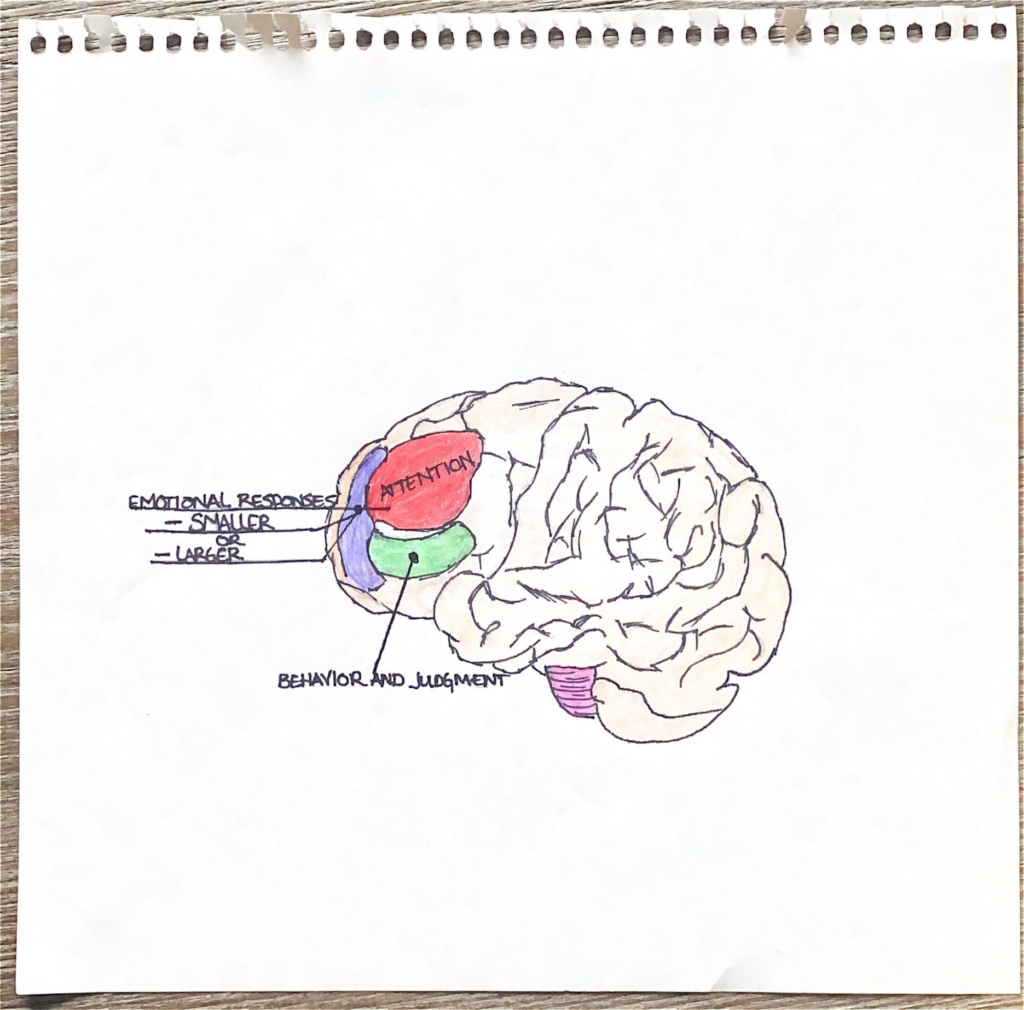
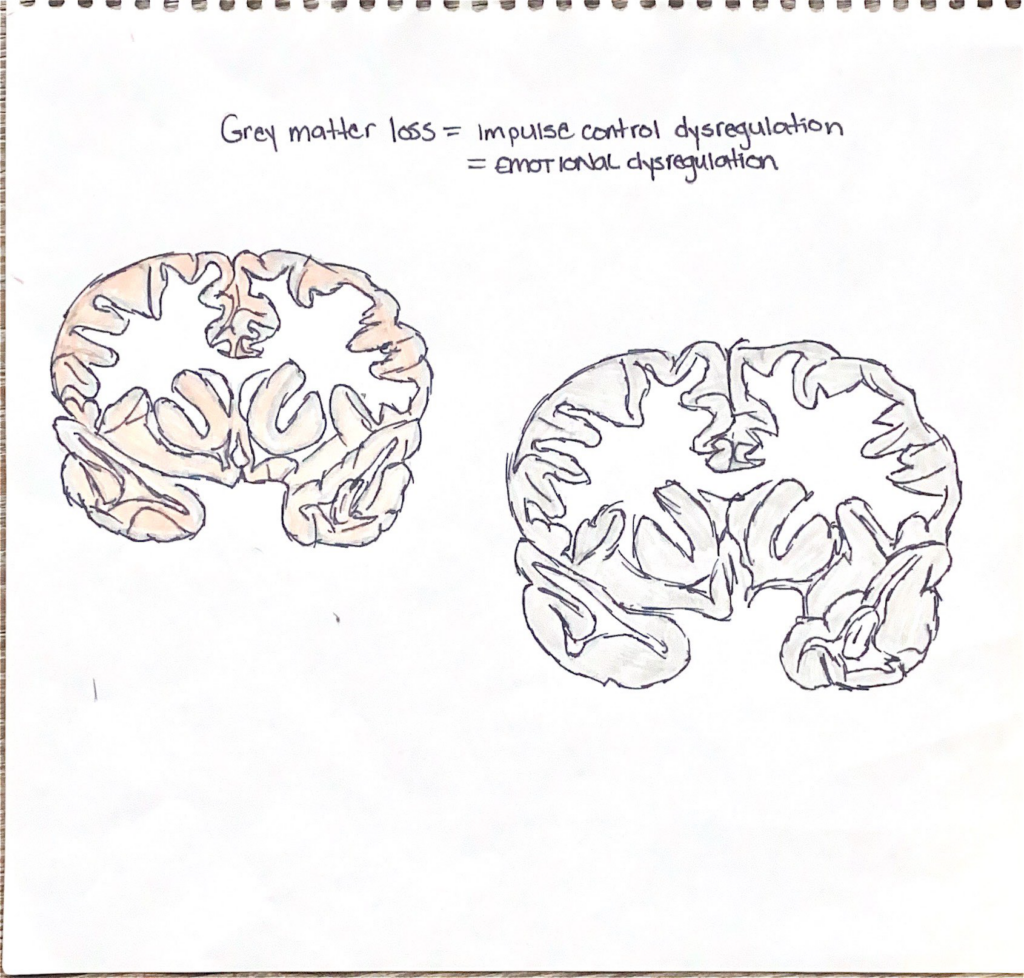
“Bipolar Disorder is associated with anatomical abnormalities of the frontal lobe.” Why is this significant? The Frontal lobe encompases the prefrontal cortex which is responsible for cognitive control functions,influencing attention and impulse inhibition.” Therefore cognitive function ties into regulating emotion. Patients are found to lose gray brain matter as well. “More gray matter seemed to indicate more self-control” Although the study of Bipolar Disorder and the effects on the brain is relatively new, there are studies that have been able to capture a glimpse how this disorder influences and distorts the brain. There are treatment options that allow individuals to lead healthy lives, the key being early diagnosis and appropriate treatment.
REFERENCES:
Benazzi, Franco. “Symptoms of Depression as Possible Markers of Bipolar II Disorder.” Progress in Neuro-Psychopharmacology and Biological Psychiatry, vol. 30, no. 3, 2006, pp. 471–477., https://doi.org/10.1016/j.pnpbp.2005.11.016.
Goodwin, Frederick King, et al. “Introduction .” Manic-Depressive Illness: Bipolar Disorders and Recurrent Depression, Oxford University Press, New York, 2007.
Baldessarini, Ross J., et al. “Age at Onset versus Family History and Clinical Outcomes in 1,665 International Bipolar-I Disorder Patients.” World Psychiatry, vol. 11, no. 1, 2012, pp. 40–46., https://doi.org/10.1016/j.wpsyc.2012.01.006.
Recognition and Diagnosis of Bipolar Disorder. https://www.psychiatrist.com/wp-content/uploads/2021/02/16856_recognition-diagnosis-bipolar-disorder.pdf.
Rajkowska, Grazyna, et al. “Reductions in Neuronal and Glial Density Characterize the Dorsolateral Prefrontal Cortex in Bipolar Disorder.” Biological Psychiatry, vol. 49, no. 9, 2001, pp. 741–752., https://doi.org/10.1016/s0006-3223(01)01080-0.
Rajkowska, Grazyna, et al. “Reductions in Neuronal and Glial Density Characterize the Dorsolateral Prefrontal Cortex in Bipolar Disorder.” Biological Psychiatry, vol. 49, no. 9, 2001, pp. 741–752., https://doi.org/10.1016/s0006-3223(01)01080-0.
Adler, Caleb M., et al. “Changes in Gray Matter Volume in Patients with Bipolar Disorder.” Biological Psychiatry, vol. 58, no. 2, 2005, pp. 151–157., https://doi.org/10.1016/j.biopsych.2005.03.022.
Saplakoglu, Yasemin. “The Amount of Gray Matter in Your Brain May Predict If You’ll Stick to Your Diet.” LiveScience, Purch, 5 June 2018, https://www.livescience.com/62744-gray-matter-brain-predict-diet-success.html.

Great job with the visual representation of the different parts of the brain and what they control as it relates to your topic!
Bipolar disorder and other mental health disorders are complex and often misunderstood. Misconceptions and misinformation on these disorders, as well as the vast range of symptoms, severity and onset, oftentimes leads to misdiagnosis. Symptoms include emotional dysregulation, impulsivity, and risky behavior. The brain is a key structure of the nervous system, and physical changes of the brain are seen in those with bipolar disorder. Specifically, bipolar disorder is associated with abnormalities of the frontal lobe, which is responsible for cognitive control functions. These cognitive control functions ultimately influence attention and impulse. There is also a connection between bipolar disorder and the loss of gray matter, which is related to self-control and information processing. Early diagnosis and appropriate treatment can help those diagnosed with bipolar disorder to live healthy lives, and aid in suppressing symptoms.
Very good read
Very good read