Natalie Clough
BIOL 112
Summer 2023
Endometriosis
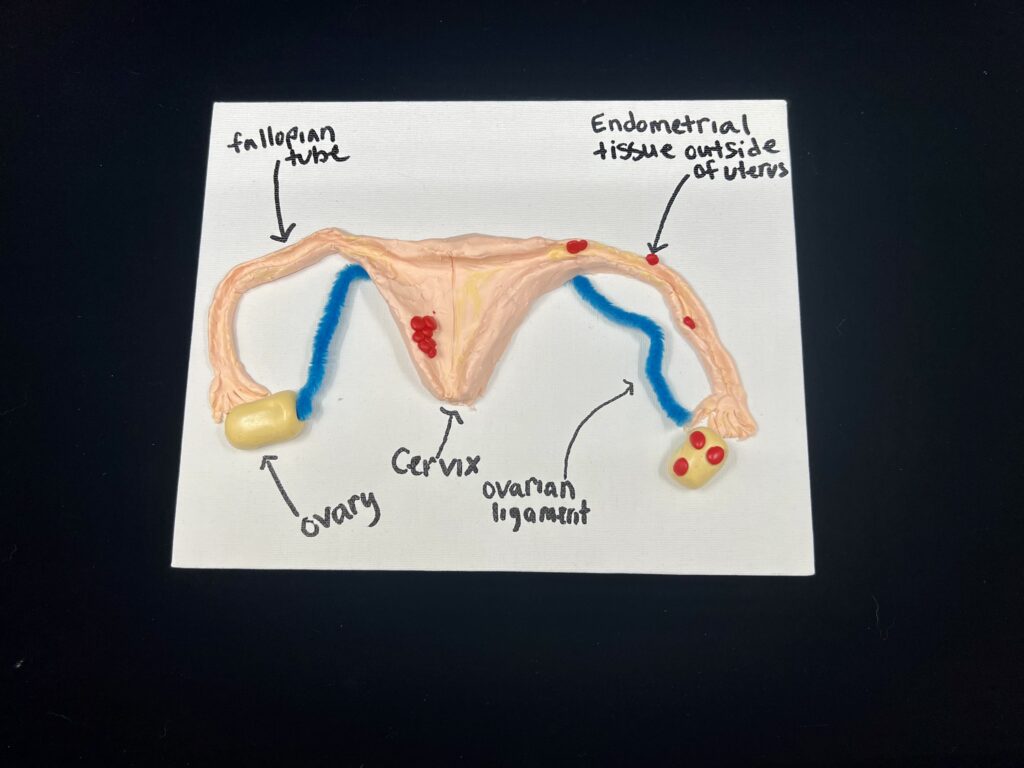
The innermost layer of the uterus is the endometrium. It consists of a connective tissue lining and epithelial tissue. This tissue provides a perfect site for implantation of an egg. If that doesn’t occur, the endometrium thins and dies and is shed from the body during menstruation. Sometimes this tissue can grow outside the uterus on other reproductive organs like the fallopian tubes, ovaries, and uterosacral ligaments. It can even be found on the bowels and outside of the pelvic region (World Health Organization, 2023). In some rare cases, endometriosis can be found as far as the diaphragm. As most women know, menstruation can be painful. In endometriosis, the pain can be severe and can make it harder to get pregnant (World Health Organization, 2023). Unfortunately, this is a chronic disease and there is no known cure at this time. Treatment is usually aimed at controlling the symptoms associated with endometriosis. Some symptoms are pain in the pelvis which can be during a period, during or after sex, or when urinating or defecating, heavy bleeding during periods, trouble getting pregnant, fatigue, depression, or anxiety (World Health Organization, 2023). Endometriosis can cause inflammation and scar tissue in the body. Since the symptoms are so variable and broad, health care workers may not be able to easily diagnose endometriosis. Some people might not have any symptoms at all.
There are many different factors that are thought to lead to endometriosis, although there is no definitive cause. Sometimes menstrual blood that contains endometrial cells can flow back into the fallopian tubes and into the pelvic cavity during the time blood is flowing out the body. This is called retrograde menstruation and it can result in endometrial-like cells being implanted outside the uterus where they can grow (World Health Organization, 2023). It is also thought that estrogen plays a huge role in endometriosis, as it can increase the inflammation and pain. Cells can sometimes change from one form to another, this is called cellular metaplasia. Cells that are outside the uterus can change into endometrial cells.
Currently, the only way to accurately diagnose endometriosis is to do laparoscopic diagnostic surgery. Once a laparoscopy is performed, histologic verification can be performed to confirm diagnosis. According to (Axelsson, Hedlund, & Fridell, 2023), MRI or magnetic resonance imaging can detect nodules and cysts that are pathological signs leading to endometriosis. This can be done preoperatively if deep endometriosis is suspected in a patient. Possible endometriosis can be found using transvaginal ultrasound technology. According to (Rozati, Khan, Mehdi, Tabasum, & Begum, 2023), oncomiR-21 can potentially detect endometriosis that can turn malignant. This is important for early detection and early treatment.
For now, treatment consists of controlling the symptoms of endometriosis. This can include removal of lesions laparoscopically; however, they can grow back. Another treatment is hormonal birth control which helps to control the pain associated with endometriosis. NSAIDS and painkillers can help control pain as well. Raising awareness can also prompt early diagnosis and slow the progression of the disease. This will reduce long term symptoms. Hopefully in the future there will be a cure for this painful and debilitating disease.
Works Cited
Axelsson, T., Hedlund, E., & Fridell, K. (2023). “But It Is Only Menstrual Pain”-A Systemic Literature Study on Diagnosis in Endometriosis. Journal of Radiology Nursing, 106-113.
Rozati, R., Khan, A. A., Mehdi, G. A., Tabasum, W., & Begum, S. (2023). Circulating oncomiR-21 as a potential biomarker of mild and severe forms of endometriosis for early diagnosis and management. Gene Reports, 1-40.
World Health Organization. (2023, 3 24). Endometriosis Fact Sheet. Retrieved from World Health Organization: https://www.who.int/news-room/fact-sheets/detail/endometriosis

Natalie did her project on Endometriosis. The endometrium is the innermost layer of the uterus consisting of connective and epithelial tissue. This tissue becomes the site for implantation of an egg. If that doesn’t occur, the endometrium will thin and dies, and will subsequently shed from the body during menstruation. This tissue can grow outside the uterus on other reproductive organs like the fallopian tubes, ovaries, and uterosacral ligaments. It can even be found on the bowels and outside of the pelvic region and in extreme cases even found as far as the diaphragm. Endometriosis is a chronic diseases characterized by chronic pain, difficulty getting pregnant, pain in the pelvis during period, during or after sex, or when urinating or defecating, heavy bleeding during periods, fatigue, depression, or anxiety. There is no definitive cause for endometriosis, but factors like retrograde menstruation and estrogen are thought to play roles in the prevalence of endometriosis. Endometriosis can be accurately diagnosed through laparoscopic diagnostic surgery. Endometriosis doesn’t have a cure but instead is treated through alleviating the symptoms of endometriosis.