Chronic pain is long standing pain that persists beyond the usual recovery period or occurs along with a chronic health condition. The cause of chronic pain is not always due to tissue damage but may also be caused by hyperactivity or disfunction of nerves either in the central nervous system or peripheral nervous system. The current treatment of chronic pain relies on the use of a drug class identified as opioids; while historically effective these drugs maintain a high affinity for addiction and tolerance due to use, and new research indicates certain people may possess a genetic predisposition for addiction to opioids. The focus of this research is to develop new methods of treating chronic pain with agonists, a substance that initiates a physiologic response when combined with a receptor, in this case pain receptors or nociceptors to replace the use of opioids in treatment of chronic pain.
The agonist compounds at the focus of this research are non-opioid and bind to the G protein-coupled receptor (GPCR) known as Alpha 2A– adrenergic receptor (α2AAR) which is a nociceptor, a receptor sensitive to pain causing stimuli, and part of the pre-synaptic adrenergic side of the autonomic nervous system. This receptor has been found to have pain-relieving effects when activated by binding norepinephrine and/or epinephrine and in turn affects central nervous system responses, such as attenuation of pain perception. So, when nor-epi binds to this receptor it inhibits the pain signal from reaching the brain and you “feeling” the pain. Note, α2AAR is not the compound, what binds to it is the focus of this research. Currently, drugs such as clonidine and dexmedetomidine are primary analgesics, or drugs that act to relieve pain, when we don’t want to use opioids; however, these drugs while not opioids and bind with the α2AAR are both heavily sedating, limiting their use to hospitals and inpatient clinics with qualified medical staff. This also means that when the patient takes the drugs to relieve their chronic pain it inhibits their ability to do day to day tasks. The researchers at the focus of this study used the ZINC15 library which is a database of commercially-available compounds for virtual screening. In this case they used it to find compounds that were dissimilar from clonidine and dexmedetomidine but still activated α2AAR, 48 high ranking compounds were selected for a process known as de novo synthesis or the synthesis of complex molecules from simple molecules such as amino acids or sugars. From this, two compounds labeled “9087” and “PS75” both acted as strong agonists of α2AAR, other compounds have also showed great promise, these two were notable in their efficacy to the research team. These compounds along with others acted in a more favorable manner because instead of acting on a broad set of G proteins such as dexmedetomidine, they only acted on Gi, Go, and Gz protein subtypes. This is important because this selective activation of cellular pathways allows for a more exact interaction in the body with less of a chance of unwanted side effects such as with clonidine and dexmedetomidine which have the unwanted effect of sedation. In lab testing, the physical characteristics of these compounds led to high brain concentrations after systemic dosing. Systemic dosing refers to the dose required for the entire body to be affected. Following systemic dosing these agonists relieved pain behaviors in neuropathic, inflammatory, and acute thermal nociception assays, or tests to determine the presence, quantity, and functional activity of a drug. Reversal of receptor binding confirmed that pain relief primarily occurred in the α2AAR, confirming that the compound was working as desired. Most importantly however, when compared with dexmedetomidine, none of the new compounds caused sedation, even at substantially higher doses than what was required for pain relief. What does this mean in plain words? These agonist compounds inhibit the stimulation/ overstimulation of pain receptors in the autonomic nervous system that send pain signals when there is no reason for or way to relieve the pain stimuli by binding to the α2AAR and sending the “feel good” or no pain signal instead of the pain signal.
So, just to recap; current methods of chronic pain management include the use of opioid which have addictive properties, and you can build a tolerance to after chronic use. The other current method involves the use of sedatives such as clonidine and dexmedetomidine that, as their name indicates, will sedate you inhibiting daily life functions. The compounds that are being tested, 9087 and PS75 among others do not sedate and are non-opioid which is very promising, and they require less of the drug than equivalent levels of opioids or sedatives to achieve the same therapeutic effect. The research is still ongoing into these compounds, and they are not available for use yet, but they do offer us promising leads into treatment of chronic pain without the use of opioids or sedatives.
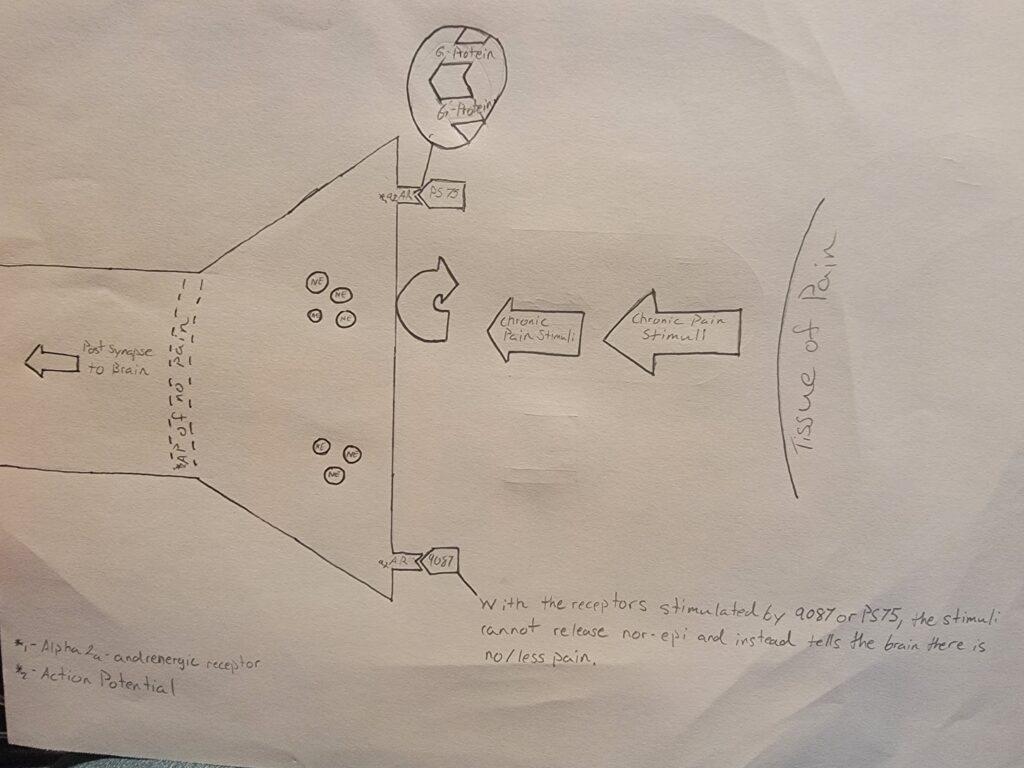
A simple visual aid to help understand the way that chronic pain is inhibited.

Shea’s steam project is on chronic pain and chronic pain therapy. The cause of chronic pain can be tissue damage, or hyperactive or dysfunctional nerves. the current treatment for chronic pain is opioids. But while very effective with helping chronic pain opioids have a terrible history of addiction and abuse. And some people even have a genetic predisposition to opioid abuse. As a result replacements for opioids are being researched. Shea’s paper focused on therapies involving agonists, initiates a response with pain receptors as a new drug for chronic pain. Agonist substances bind gpcr to a pain receptors. This specific brain receptor is known to cause pain relief effects when activated. drugs that bond to this pain receptor are what’s being researched for this pain therapy. two of these drugs are particularly successful. these are 9087 and ps75. these compounds act with a lot of the gpcr. systemic dosing of these drugs provided great relief from neuropathic, inflammatory, and acute thermal nociception assays. tic along with reversal of receptor binding Showns that these drugs give desired results. so the agonist blocks the pain signals. while these compounds are not available yest they are promising for the world of medicine. Sheas objective that related to this topic was compare and contrast the central nervous system and the peripheral nervous system. this topic really delved into how these nervous system function regarding sensing pain. it was also an interesting topic with lots of good research ang science. great job with this steam project.