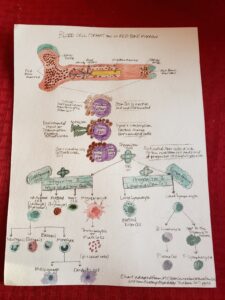
One of the 7 functions of bones is blood formation or hematopoiesis. In adults this takes place in the red bone marrow. For my STEAM project I wanted to learn about and then display the process a stem cell goes through in the bone marrow of becoming a blood cell or lymph cell. I drew and painted a flow chart of the (purple) stem cell surrounded by (red) niche cells that eventually receive a (green) signal that begins the transformation of the stem cell to divide and create a (teal green) progenitor cell 1 or 2 that will specialize into either a blood or lymph cell. The flow chart then shows how each of the blood forming cells eventually can become white, red, mast, or megakaryocyte cells that specialize further. And the lymph forming cells eventually become large or small lymphocytes and then specialize more. I then created a mobile with bones and playdough and pompoms attempting to follow the flow chart of these blood and lymph cells. In my paper I went into a bit more about some factors that influence the nice surrounding the stem cell that helps in deciding what the cell will eventually become. It was a very fascinating study and it made me want to learn more about stem cells and the role they play in healing in the body.
Class objective: Identify the 7 functions of bone. One of the 7 functions of the bone is blood formation.
Stem cells are a type of unspecialized “master” cells that don’t have any defined job, function, or structure but have the potential to turn into any cell in the body as needed. This is called differentiating into specialized cells and the body uses it to grow, regenerate, and replace damaged and worn out cells as needed. In this Steam project, I focused on the hemapoietic stem cells in the red bone marrow of an adult that specialize to create blood and lymph cells. The process of creating blood in the bone marrow has the fancy name of hematopoiesis and generally gives rise to 4 distinct types of blood cells: red blood cells (erythrocytes) that help deliver oxygen throughout the body, white blood cells (leukocytes) that fight pathogens in the body, mast cells, and platelets (thrombocytes) that help clot the blood during an injury.
Bone marrow is found in your bones throughout your body. The bone marrow is spongy and viscous. There are 2 types of bone marrow. The first is red bone marrow, a highly vascularized, delicate, and fibrous tissue at the end of long bones or in other bones like ribs, vertebrae, sternum, skull, and the pelvis that stores immature cells called hematopoietic stem cells that produce around 500 billion blood cells a day. The second type is yellow bone marrow located under the compact bone and in the shaft of long bones and stores fat and contains mesenchymal stem cells also called stromal cells that eventually produce fat, cartilage, and bone cells.
The undifferentiated hematopoietic stem cells (HSC) live surrounded by cells and proteins that maintain them in a quiescent or inactive state and keep them undifferentiated. This cellular environment is called a niche and is “an intricate network of cells in the bone marrow microenvironment”. (Galan-Diez, Cuesta-Dominguez, & Kousteni, 2018, p. 1) When an activation occurs (say you cut yourself) or a signal is sent that more red blood cells need to be replaced in the body, an environmental input or some transcription factors will activate cells surrounding the stem cell to change. It’s this environmental influence from the niche that begins the differentiation process to turn the stem cell into the specific cell needed. This change in the niche is what causes the stem cell to differentiate. Certain proteins are bound or stop inhibiting the stem cell and specific genes in the DNA are turned on or off, regulating the stem cells genetic expression as it begins the process of specializing. An example of one of these important proteins that signals a stem cell to specialize is the G-CSF Granulocyte-Colony Stimulating Factor. This G-CSF stimulates the bone marrow stem cells to become white blood cells called neutrophils. Remember the stem cell has the latent potential (all of the DNA) to become any cell needed, so selectively turning genes on and off establishes the path of differentiation or specialization that the cell will take. This will cause the stem cell to specialize to become the specific cell that is needed. Once stimulated, the hematopoietic stem cells begin to divide. The activated stem cell will usually first make an exact duplicate of itself or a new stem cell and then one daughter cell called a progenitor cell that will be the one to specialize. This clever process ensures the stem cell numbers stay strong by constantly replacing itself, creating an endless and regenerative cycle. When the HSC makes the daughter cell, this is the beginning of differentiation, and it will choose to make a progenitor 1 daughter cell that is a myeloid stem cell and creates blood cells or it will make a progenitor 2 daughter cell that is a lymphoid stem cell and create an immune cell. The myeloid stem cell (progenitor 1) will continue to specialize eventually forming red blood cells, platelets, mast cells, or white blood cells (basophils, neutrophils, eosinophils, monocytes, macrophages, and dendritic cells). For example, if a progenitor 1 or myeloid cell commits to becoming a proerythroblast, it will develop into a brand-new red blood cell. Whereas the lymphoid stem cells (progenitor 2) will continue to differentiate forming more white blood cells for the immune system by first differentiating between large lymphocytes and small lymphocytes. The large granular lymphocytes eventually produce Natural Killer cells. The small lymphocytes further specialize forming B-lymphocytes or T-lymphocytes. The B-lymphocytes will eventually become plasma cells, but the immature T-lymphocytes are sent to the thymus to finish their maturation process. It is interesting to note that either route the differentiated stem cell takes (myeloid or lymphoid) white blood cells can emerge. All of this specialization and differentiation of the blood and lymph cells is dependent on the type of stimulus the stem cell receives from its niche so it can know how to differentiate.
I really enjoyed learning about the stem cell potential and the fascinating process of how they are stimulated to become differentiated and specialized cells. I would really enjoy going more in depth in this subject to learn about what the exact transcription factors are that influence the stem cell to specialize and if there are nutrients that encourage this process more. I think I would enjoy learning more about Regenerative Medicine where their goal is to repair damaged tissue in the body using a person’s own stem cells. I would love to learn more about the healing and regenerative options available with stem cells and also if there is a way to increase a person’s own stem cell production though nutrition.

Bibliography:
Betts, J.G., Desaix, P., Johnson, J.E., Korol, O., Kruse, D., Poe, B., Wise, J.A., Womble, M., & Young, K.A. (2017). Anatomy and Physiology. Houston, Texas. OpenStax Rice University.
Pinho, S., Frenette, P. S. (2019 May) Haematopoietic stem cell activity and interactions with the niche. Nat Rev Mol Cell Biol. 20(5), 303-320.
Galan-Diez, M., Cuesta-Dominguez, A., & Kousyeni, S. (2018, July). The bone marrow microenvironment in health and myeloid malignancy. Cold Spring Harb Perspect Med. 8(7): a031328.
Nichols, H. (2017, December 15). All you need to know about bone marrow. Medical News Today.
MIT OpenCourseWare. (2014, January 15). Introductory biology, Lecture 23: Stem cells [YouTube video]. MIT. Retrieved from https://www.youtube.com/watch?v=62FdhX-zS2Y.

With Lori Beckdahl’s project, she covered the objective of the one of the functions of the bone, which is blood formation. She discusses the two types of bone marrow, and how her objective covers specifically the STEM cells in the red bone marrow. She displays her objective through an organized flowchart which showcases where the STEM cells are located in the red bone marrow in the bone, and the process of the STEM cell transitioning from inactive to active. When the STEM cells are activated, Lori demonstrates how the STEM divide and produces progenitor daughter cells. The first daughter cell is named the myeloid stem cell which creates the main blood cells known as the white blood cell, red blood cell, mast cell, and megakaryocyte. The progenitor 2 daughter cell produced are the lymph forming cells and are known as lymphoid STEM cell. These cells can be classified as the large lymphocyte cell and the small lymphocyte cell. The lymphoid STEM cell functions to create an immune cell that will benefit and strengthen the immune system. With Lori’s flowchart, she also showcases the classification of these specialized cells through a 3-D diagram which was very neat and well represented. She used a real bone to showcase the bone and used all sorts of sphere-shaped objects to represent the specialized cells. I think Lori did an amazing job with her project. I found this topic very interesting and her research was very well-informed discussing these specialized cells that are useful to our bodies. Science continues to discover new ways to use these cells, and it will be interesting to see their new discoveries for regenerative medicine with these STEM cells throughout the following years.